Items filtered by date: August 2022
When Older Adults Experience Heel and Back-of-the-Foot Pain
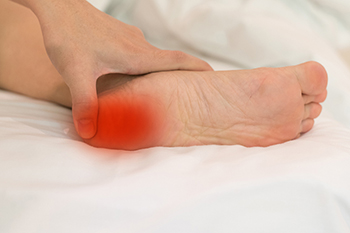
Older adults are at an increased risk of developing foot problems. If you have heel pain or pain that is located at the back of your feet, chances are that it may be one of three conditions: plantar fasciitis, bursitis, or an Achilles tendon injury. Plantar fasciitis is the most common form of heel pain. This occurs when the plantar fascia tissue on the bottom of the foot gets injured or irritated and inflamed, typically through overuse. Plantar fasciitis pain is usually more intense in the morning or after periods of rest. Your podiatrist may treat it with custom orthotics, physical therapy, corticosteroid injections, shockwave therapy, or by other means. Bursitis is an inflammatory condition that affects the bursa sac between your Achilles tendon and heel bone at the back of your foot. This is a fluid filled sac that cushions joints and bones, helps protect the tendon, and reduces friction. This bursa can become inflamed, painful, swollen, or red from repetitive motions or direct pressure. The Achilles tendon can suffer from various injuries such as ruptures, tendonitis, or enthesopathy, which are typically caused by intense or repetitive strain on the tendon. If you feel any of the symptoms described here, have a podiatrist examine you and perform whatever tests are necessary to properly diagnose your condition and devise an effective treatment plan.
Many people suffer from bouts of heel pain. For more information, contact Nrup Tolat, DPM of Atlanta Total Foot & Ankle Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Causes of Heel Pain
Heel pain is often associated with plantar fasciitis. The plantar fascia is a band of tissues that extends along the bottom of the foot. A rip or tear in this ligament can cause inflammation of the tissue.
Achilles tendonitis is another cause of heel pain. Inflammation of the Achilles tendon will cause pain from fractures and muscle tearing. Lack of flexibility is also another symptom.
Heel spurs are another cause of pain. When the tissues of the plantar fascia undergo a great deal of stress, it can lead to ligament separation from the heel bone, causing heel spurs.
Why Might Heel Pain Occur?
- Wearing ill-fitting shoes
- Wearing non-supportive shoes
- Weight change
- Excessive running
Treatments
Heel pain should be treated as soon as possible for immediate results. Keeping your feet in a stress-free environment will help. If you suffer from Achilles tendonitis or plantar fasciitis, applying ice will reduce the swelling. Stretching before an exercise like running will help the muscles. Using all these tips will help make heel pain a condition of the past.
If you have any questions please contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Wounds That Don't Heal Need to Be Checked
Why Does Gout Develop?
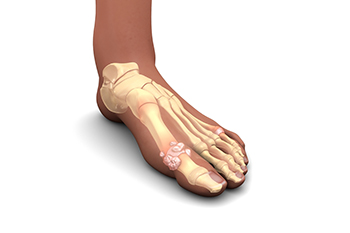
A form of arthritis known as gout can cause severe pain and discomfort and many people have difficulty in walking. Gout develops because of excess uric acid in the blood and may result from genetic factors or eating foods that have high levels of purines. These foods can include shellfish, red meat, alcohol, or drinks that are made with large amounts of sugar. This can cause crystals to develop in the joints of the big toe and may cause debilitating pain as well as redness and swelling. For many people, maintaining a healthy eating regimen can limit the number of gout attacks. It can help to drink plenty of fresh water daily and to engage in a gentle stretching and exercise program. It is beneficial to find out why they may be recurring and learn about methods to control them. If you have gout, it is strongly advised that you are under the care of a podiatrist who can guide you toward correct treatment options and educate you about effective preventive methods.
Gout is a painful condition that can be treated. If you are seeking treatment, contact Nrup Tolat, DPM from Atlanta Total Foot & Ankle Care. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Where Is the Plantar Fascia?
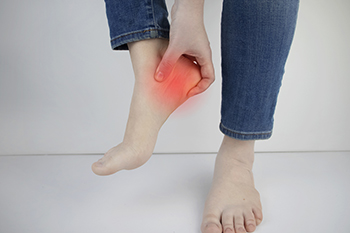
The condition plantar fasciitis exists when the plantar fascia becomes inflamed. It is the band of tissue that is found on the bottom of the foot that can become torn or damaged from a foot injury. Additionally, it may happen from standing for most of the day, or from frequently walking on hard surfaces. Many people experience general foot pain with plantar fasciitis, and the foot may feel stiff and tender. It is beneficial to adjust daily living activities, and to temporarily stop doing what caused the pain. There are patients who find mild relief when specific foot exercises and stretches are performed, in addition to possibly wearing orthotics in their shoes. In severe cases, surgery may be a necessary option to repair the damaged portion of tissue. If you have heel pain, please confer with a podiatrist who can properly diagnose plantar fasciitis, and offer you correct treatment advice.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Nrup Tolat, DPM from Atlanta Total Foot & Ankle Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Healing Plantar Dermatosis in Kids

A condition called juvenile plantar dermatosis is a fancy term for dry skin on the feet. It usually affects children between the ages of 3 and 14 and is most prevalent around the age of 8. It rarely affects adults and diminishes in children when they reach puberty. Causes include friction from the sole rubbing inside the shoe, wearing synthetic shoes or shoes that do not “breathe,” and excessive sweating followed by rapid drying that leads to cracks in the skin. With plantar dermatosis, the soles of the feet typically become red, shiny, itchy, or sore and take on a glazed appearance. It usually affects both feet starting with the big toe and results in painful fissures, cracking, and scaling. For this reason, it may be confused with athlete’s foot or eczema. Treatment includes wearing shoes that fit well and are not made of leather or plastic, avoiding synthetic socks, and applying moisturizing cream daily. To find out more about plantar dermatosis in your child, please consult a podiatrist who can rule out other causes and prescribe the appropriate medication.
The health of a child’s feet is vital to their overall well-being. If you have any questions regarding foot health, contact Nrup Tolat, DPM of Atlanta Total Foot & Ankle Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Tips for Keeping Children's Feet Healthy
- Make sure their shoes fit properly
- Look for any signs of in-toeing or out-toeing
- Check to see if they have Clubfoot (condition that affects your child’s foot and ankle, twisting the heel and toes inward) which is one of the most common nonmajor birth defects.
- Lightly cover your baby’s feet (Tight covers may keep your baby from moving their feet freely, and could prevent normal development)
- Allow your toddler to go shoeless (Shoes can be restricting for a young child’s foot)
- Cut toenails straight across to avoid ingrown toenails
- Keep your child’s foot clean and dry
- Cover cuts and scrapes. Wash any scratches with soap and water and cover them with a bandage until they’ve healed.
If you have any questions, please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
All About Diabetic Foot Ulcers
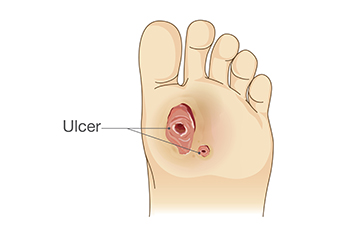
A diabetic foot ulcer is an open sore or wound that affects about 15 percent of people with diabetes. There are two main types of foot ulcers, neuropathic and vascular. High blood sugar levels are thought to be the cause of both types. Being overweight, smoking, and frequently drinking alcohol are other contributing factors. People who have diabetes for years often develop neuropathy, a reduced or limited ability to feel pain in the feet. As a result, sores and cuts, especially on the bottom of the feet, may be overlooked. Vascular inefficiency, a slowed blood flow to the extremities, can reduce the ability of foot ulcers to heal properly, which increases the likelihood of infection. Tissue around a skin ulcer can become blackened, and gangrene may develop. Of those who develop a foot ulcer, up to one-fourth will be at risk of amputation. Fortunately, it is possible to prevent the formation of foot ulcers through a rigorous daily foot care regime. If an ulcer has formed, however, debridement (cutting away of dead tissue), certain medication, sterile dressings, and managing glucose are suggested. For more information on prevention and treatment of foot ulcers, please consult a podiatrist.
Diabetic foot care is important in preventing foot ailments such as ulcers. If you are suffering from diabetes or have any other concerns about your feet, contact Nrup Tolat, DPM from Atlanta Total Foot & Ankle Care. Our doctor can provide the care you need to keep you pain-free and on your feet.
Diabetic Foot Care
Diabetes affects millions of people every year. The condition can damage blood vessels in many parts of the body, especially the feet. Because of this, taking care of your feet is essential if you have diabetes, and having a podiatrist help monitor your foot health is highly recommended.
The Importance of Caring for Your Feet
- Routinely inspect your feet for bruises or sores.
- Wear socks that fit your feet comfortably.
- Wear comfortable shoes that provide adequate support.
Patients with diabetes should have their doctor monitor their blood levels, as blood sugar levels play such a huge role in diabetic care. Monitoring these levels on a regular basis is highly advised.
It is always best to inform your healthcare professional of any concerns you may have regarding your feet, especially for diabetic patients. Early treatment and routine foot examinations are keys to maintaining proper health, especially because severe complications can arise if proper treatment is not applied.
If you have any questions please feel free to contact our offices located in Woodstock and Atlanta, GA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

